 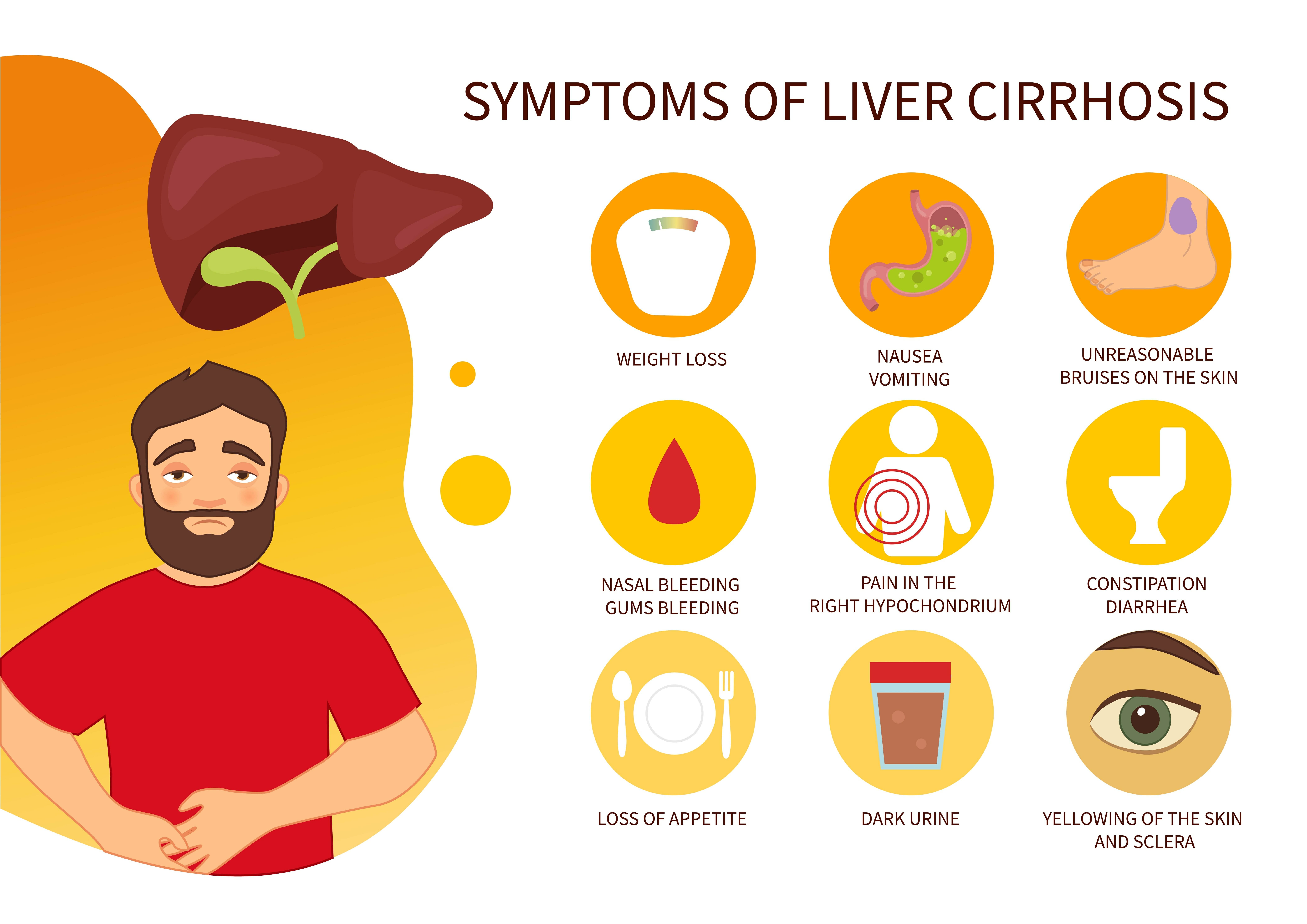
16– 18 Therefore, it seems essential to rely on both subjective and objective methods to obtain a global picture of sleep in patients. This is due to the fact that patients, especially insomniacs, tend to underestimate their sleep quality. It should also be emphasized that correlations between subjective and objective sleep disturbances are not strong. 
Objective methods classically applied in the sleep lab, such as polysomnography (PSG) and actigraphy, allow more precise assessment. Subjective tools, such as questionnaires and sleep logs, can be used to collect sleep quality and daytime complaints. The reported prevalence of sleep–wake abnormalities in cirrhosis depends upon the diagnostic tools used to assess them. 14, 15Ĭharacteristics and prevalence of sleep disturbances in liver cirrhosis Other common sleep disorders, such as obstructive sleep apnea syndrome or restless legs syndrome, are also more prevalent in patients with liver cirrhosis and will not be discussed in the present review. 11 Etiology of cirrhosis does not influence the occurrence/the clinical picture of sleep disturbances that have been observed both in series of patients affected exclusively or mainly by hepatitis C 2, 10, 11, 12 and in series including a majority of alcoholic cirrhosis. 10 Comparison of sleep in cirrhosis with prior HE vs without prior HE has also highlighted a further deterioration of sleep quality, with more non-restorative sleep. Indeed, Bajaj et al have observed EDS and poor quality of sleep in compensated cirrhotics compared to healthy controls. 
If most sleep disturbances in cirrhotic patients are attributed to HE, 9 sleep disturbances seem to be already present in compensated cirrhosis. 4 This was first described in 1954, by Sherlock et al, as a phenomenon of “sleep–wake inversion.” 8 The most common abnormalities include insomnia (difficulty falling asleep or maintaining sleep, or unrefreshing sleep), excessive daytime sleepiness (EDS), and sleep–wake inversion (disturbances of circadian rhythmicity). In these patients, sleep disorders have serious implications for daytime functioning and are best described as a panel of sleep–wake abnormalities. 6 In a recent study by Singh et al, 7 32% of patients with liver cirrhosis exhibited HE. 
In recent American and European guidelines, altered sleep rhythm is an essential factor in the diagnosis of HE. 5 Diagnosis of HE still remains difficult and is primarily based on clinical findings. HE has a broad spectrum of clinical severity, ranging from subclinical disorders (covert) to overt HE with coma. Sleep disturbances in liver cirrhosis are closely related to the presence of HE. However, due to the potential for medication toxicity in these disabled patients, further studies are needed to address the potential role of non-drug therapies in this population (eg, cognitive behavioral therapy, mindfulness, yoga) that have demonstrated usefulness in insomnia disorders.Ĭlinical manifestations of sleep disturbances in liver cirrhosis A few non-specific treatments for sleep–wake abnormalities have been tried with encouraging results for hydroxyzine and modafinil. Sleep–wake abnormalities are related to the presence of hepatic encephalopathy (HE) and improvement in sleep parameters can be observed when HE is properly managed. The underlying pathophysiological mechanisms for sleep disturbances in cirrhosis are complex and may include disturbed metabolism of melatonin and glucose, alterations in thermoregulation, and altered ghrelin secretion profiles. The most common abnormalities are insomnia (difficulties falling asleep and maintaining sleep, or unrefreshing sleep), excessive daytime sleepiness, and sleep–wake inversion (disturbances of circadian rhythmicity). Sleep–wake disturbances are common in liver cirrhosis and associated with impaired quality of life. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
